How CDS Systems Improve Quality in Value-Based Care
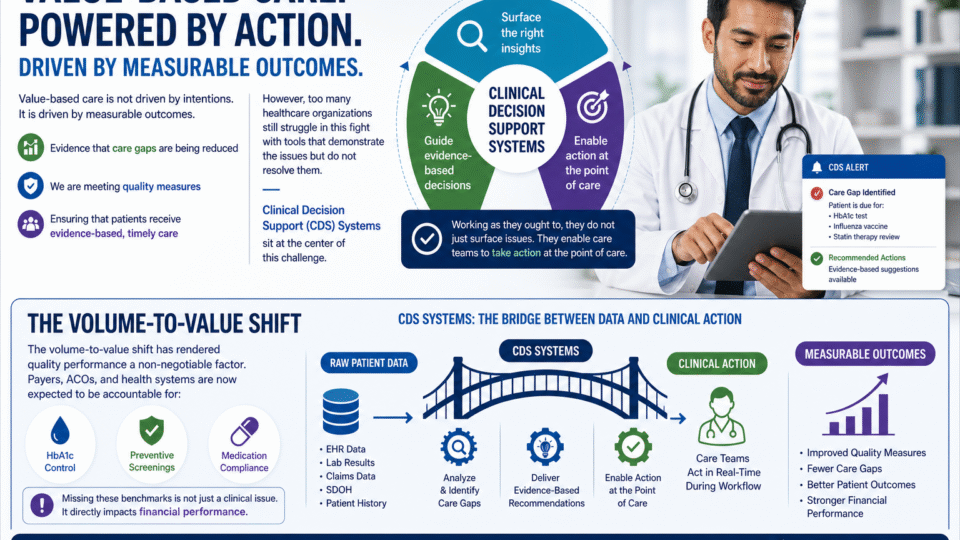
Value-based care is not driven by intentions. It is driven by measurable outcomes. Evidence that care gaps are being reduced, we are meeting quality measures, and ensuring that the patients receive evidence-based, timely care. However, there are too many healthcare organizations still struggling in this fight with tools that demonstrate the issues but do not resolve them. Clinical Decision Support CDS Systems sit at the center of this challenge. Working as they ought to, they do not just surface issues. They enable care teams to take action at the point of care.
The volume-to-value shift has rendered the quality performance as a non-negotiable factor. The payers, ACOs, and health systems are now expected to be responsible for measures such as HbA1c control, preventive screenings, and medication compliance. Missing these benchmarks is not just a clinical issue. It directly impacts financial performance. It is there that Clinical Decision Support CDS Systems come in as the bridge between data and clinical action, transforming raw patient data into tangible, quantifiable changes at the point of care.
What Role Do CDS Systems Play in Value-Based Care?
CDS systems connect clinical data to care decisions in real time, at the point of care. Quality measures are a core component of value-based care programs. All of the scores (HEDIS scores, Star Ratings, ACO benchmarks) rely on the right care occurring at the right time. CDS systems provide care teams with alerts in situations where a patient requires a screening, the management of a chronic condition is suboptimal, or a care gap is present, and in more advanced applications, they help close care gaps in real time.
Why Read-Only CDS Falls Short
Most traditional CDS tools generate alerts. That’s it. They inform a clinician that something has to be done and leave the implementation to another system, another workflow, or another day.
Here’s what that actually costs:
- 2–3 minutes lost per actionable alert due to system switching
- Clinicians are mentally tracking unresolved tasks across multiple platforms
- Care gaps that get flagged but are never formally closed in the EHR
- Quality measures that don’t get credited because the documentation was incomplete
The real issue isn’t alert volume; it’s the cognitive tax of every micro-decision that follows each alert. Clinicians don’t need more information. They need fewer decisions standing between an insight and an action.
How CDS Systems Directly Improve Quality Measure Performance
Quality measure performance improves when CDS moves from passive notification to active enablement.
Closing Care Gaps at the Point of Care
A care gap is only considered closed when it is documented in the EHR. This documentation can be completed within the same workflow, since advanced CDS systems can both read from and write back to the EHR.
Consider what this looks like in practice:
- A patient is overdue for a diabetic eye exam → CDS flags it → clinician orders the referral from the same screen → gap closes in real time.
- A medication adherence alert appears → prescription renewal is triggered immediately → care plan is updated automatically.
- An HCC code opportunity is identified → clinician captures it on the spot → no follow-up task needed.
This is the difference between a quality program that runs on spreadsheets and follow-up calls versus one that closes gaps during the encounter itself.
Reducing Cognitive Overload for Clinicians
One of the most significant barriers to quality measure performance is cognitive overload. When clinicians deal with fragmented systems and incomplete workflows, they prioritize urgent tasks, and quality documentation often gets delayed.
The core principle is simple: reduce steps instead of adding more.
The adoption increases as soon as the alerts enter the EHR workflow, not as a pop-up of an external tool but as a natural part of the existing clinical workflow.
Supporting Care Coordination Across the Team
Quality measures aren’t the responsibility of one clinician. They cut across care managers, nurses, PCPs, and specialists. Real-time CDS systems allow the entire care team to see what is completed, what is pending, and what is at risk without manual follow-ups.
This shared visibility:
- Prevents duplicate outreach to patients
- Ensures accountability is clear across roles
- Keeps care plans updated across all care settings
What Makes a CDS System Truly Effective for Quality Programs?
The most effective CDS systems share a few non-negotiable characteristics:
| Feature | Why It Matters |
| Bidirectional EHR integration | Closes gaps without leaving the primary workflow |
| Native workflow embedding | Drives adoption by reducing friction |
| Real-time data synchronization | Keeps all team members on the same page |
| HCC code capture at the point of care | Directly supports risk adjustment and quality scores |
| Multi-EHR compatibility | Works across diverse provider environments |
A digital health platform that meets these criteria actively supports and strengthens quality programs.
Takeaway
Quality measure performance in value-based care is not just a reporting issue. It is an execution issue. Systems that expose insights but do not enable action fall short of true Clinical Decision Support (CDS) systems, shifting the burden of action onto already stretched clinicians. Organizations that succeed in value-based care are those that use CDS systems that close the loop between insight and action, lessen cognitive load, and capture results directly within the point-of-care workflow.
Persivia’s CareTrak® is a point-of-care CDS platform with bidirectional connectivity across 80+ EHR systems, enabling clinicians to capture HCC codes, close care gaps, and update care plans without ever leaving their primary workflow. Integrated within the broader Persivia CareSpace® population health ecosystem, it gives care teams the real-time visibility and action capability that value-based care programs demand.











Leave a Reply